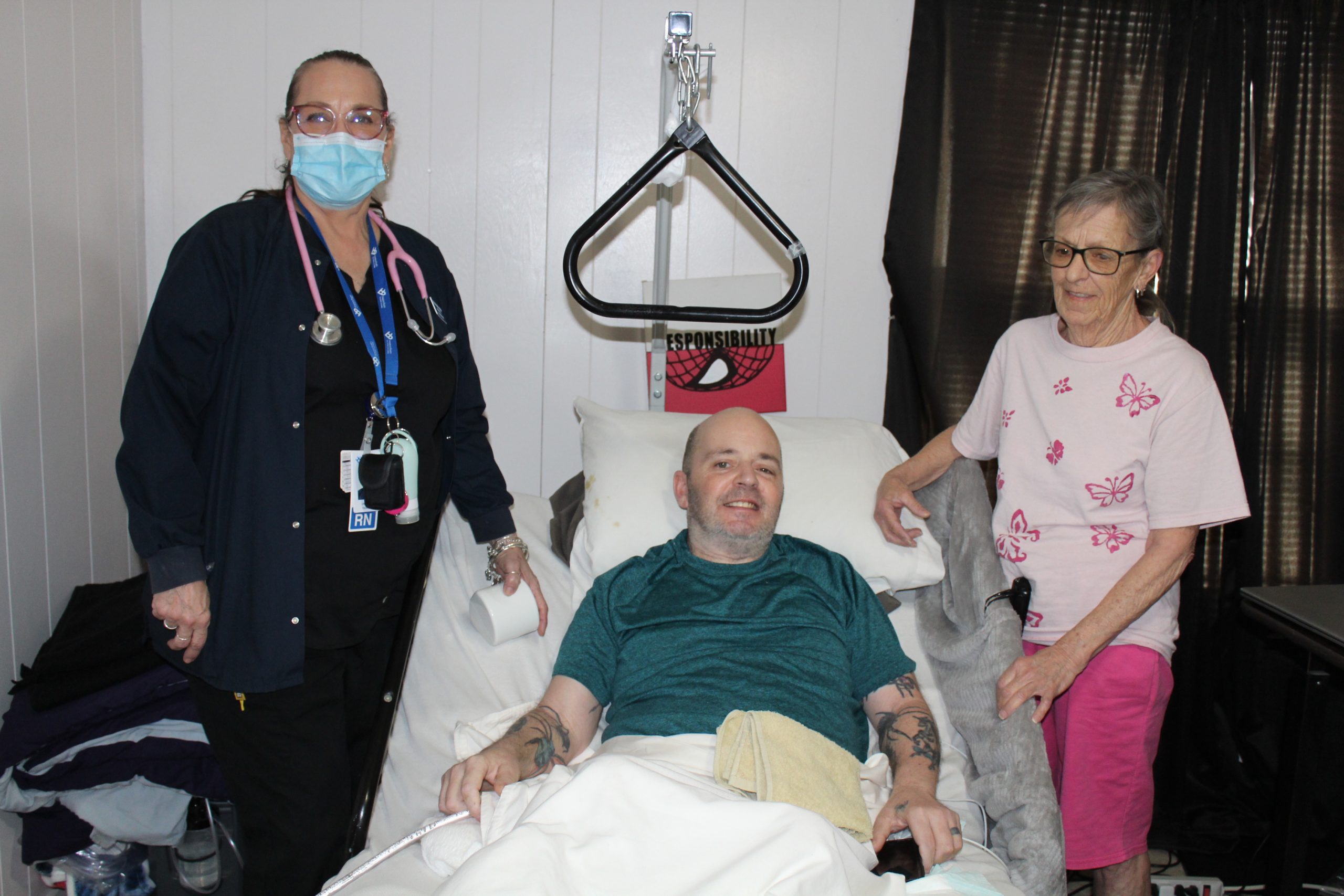
When Matt Weiss had a heart attack, he didn’t even know it. He was in his 40s, in great shape, worked out every day, rarely even ate fast food. He didn’t go to the doctor, because he didn’t have insurance. A couple of months later, his feet – and shortly later his entire body – swelled up badly with edema. He did see a doctor then, who told him to go straight to the hospital. Only 10% of his heart was working.
Matt came on to Hospice Austin’s service as an unfunded patient in February 2022. Last year, Hospice Austin provided more than $1.8 million in care to uninsured and underinsured patients, a 49% increase from the year before. While most hospices – even nonprofits – limit the number of unfunded patients they accept, Hospice Austin has never done that. Our Hospice Access for All Program (HAAP, formerly known as Charity Care) accepts all who need our services regardless of the patient’s ability to pay.
We are able to tell someone who is sick, can’t work, and has no insurance that they now have comprehensive care completely free to them through Hospice Austin – that our HAAP program will provide all medications, equipment, and care they need and it won’t cost them a dime. Their relief is always palpable.
Matt Weiss with Social Worker Shelby Thomas
Our social workers connect unfunded patients with resources to make their lives a little easier: Meals on Wheels, caregiver support, applying for benefits. Hospice Austin maintains a Special Needs Fund to help patients most in need with rent, utilities, HEB gift cards and other necessities. Matt’s Hospice Austin social worker, Shelby Thomas, worked together with his ex-wife to apply for Social Security Disability for Matt, both spending hours on hold with the SS office.
When his disability claim was recently approved and he received a lump sum of back payments, Matt told Shelby he wanted to donate 10% to Hospice Austin. He said it was the least he could do to show his appreciation and gratitude for all Hospice Austin has done for him the last year. Shelby and the rest of Matt’s team tried to talk him out of it. He and his mother, Alice, don’t have a lot – they live modestly in a small town and visit their local food bank. Matt was not to be deterred.
“Matt has such a genuine and giving soul,” Shelby said. “He said that he couldn’t think of a better way to give back than to those who’ve been giving to him. I felt a brief moment of surprise, and then I wasn’t surprised at all. He and his mom both have such giving hearts.”
Shelby brings them HEB gift cards and also items from our small food pantry. When Alice gets items at her local food bank that she doesn’t think they will use, she gives them to Shelby for Hospice Austin’s food pantry.
Shelby said it’s a blessing to have the flexibility and freedom to meet our patients’ needs. At other places she’s worked, she’s had to tell her clients no, she’s not able to help them. “Here, I’m able to say yes to so many different things,” Shelby said. “I love my job! I get to empower people and advocate for them and offer a light in such a dark time.”
Matt’s gift will help others with no insurance get the care they need, both at home and at Hospice Austin’s Christopher House, just as Matt has.
“There’s no way I could have done this without Hospice Austin’s help, so why wouldn’t I give back?” Matt asked. “I wouldn’t be here without Hospice Austin.”

Melinda Marble
Communications Coordinator